Learning medicine is hard work! Picknova makes it easy. It takes your lectures and notes to create a personalized study plan with exclusive articles, practice questions and flashcards, and so much more.
Try it free today!
Lung cancer, or lung carcinoma, is the uncontrolled division of epithelial cells that line the respiratory tract. There are two main categories of lung cancer, small cell and non-small cell, which depend on the type of epithelial cell that’s dividing.
Both types can be fatal, mainly if the cancerous cells aggressively spread and establish secondary sites of cancer in other tissues. The primary cause of lung cancer is smoking tobacco products, and it has contributed to the deaths of millions of people, including famous individuals like Walt Disney and Claude Monet.
Air enters the respiratory tract through either the nose or mouth and flows down the trachea, which divides into the right and left bronchi. Each bronchus enters its respective lung at the hilum, or root of the lung.
The bronchi then divide into lobar bronchi, which divide into segmental bronchi, then into subsegmental bronchi, which further branch to form conducting bronchioles. Then respiratory bronchioles which end with small sacs called alveoli that are surrounded by capillaries, which is where gas exchange occurs.
Lining these airways are several types of epithelial cells that serve multiple functions. These include ciliated cells that have a hair-like project called cilia that work to sweep foreign particles and pathogens back to the throat to be swallowed.
Another type, called goblet cells–which are called that because they look like goblets–secrete mucin to moisten the airways and trap foreign pathogens. There are also basal cells that are thought to be able to differentiate into other cells in the epithelium, club cells that act to protect the bronchiolar epithelium, and neuroendocrine cells that secrete hormones into the blood in response to neuronal signals.
Cells can become mutated because of environmental or genetic factors. A mutated cell becomes cancerous when it starts to divide uncontrollably. As cancer cells start piling up on each other, they become a small tumor mass, and they need to induce blood vessel growth, called angiogenesis, to supply themselves with energy.
Malignant tumors are ones that are able to break through the basement membrane. Some of these malignant tumors go a step further and detach from their basement membrane at the primary tumor site, enter nearby blood vessels, and establish secondary sites of tumor growth throughout the body – a process called metastasis.
A well-known risk factor for small cell lung cancer and some types of non-small cell lung cancer is smoking tobacco, and it’s dose-dependent, which means that smoking more cigarettes over a longer period of time increases the risk.
Another risk factor is exposure to radon, a colorless, odorless gas, which is a natural breakdown product of uranium found in the soil. Other environmental factors include asbestos, air pollution, and ionizing radiation, like from medical imaging with chest X rays and CT scans.
There are also some gene mutations that are known to be associated with an increased risk of lung cancer development. Once it develops, lung cancer tends to metastasize quickly, rapidly establishing sites of secondary tumors in other tissues.
Tissues, particularly at risk as a secondary site, in the mediastinum and hilar lymph nodes because of their proximity to the lungs, but other sites include the lung pleura – the lining of the lungs, heart, breasts, liver, adrenal glands, brain, and bones. Lung cancer can be categorized as either small cell or non-small cell carcinomas.
Small cell carcinomas account for a small portion of lung cancers and originate from small, immature neuroendocrine cells. That means that non-small cell carcinomas account for most lung cancers, and these can be further subdivided into four categories: adenocarcinomas which frequently form glandular structures or have the ability to generate mucin; squamous cell carcinomas; which have squamous, or square-shaped, cells that produce keratin; carcinoid tumors from mature neuroendocrine cells; and large cell carcinomas which lack both glandular and squamous differentiation.
Small cell carcinoma is strongly associated with smoking and usually develops centrally in the lung, near the main bronchus. In general, they grow the fastest and more rapidly metastasize to other organs than other types of non-small cell lung cancers.
Because of this, by the time it’s diagnosed, it’s common to find large tumors in multiple locations both within and outside the lung. Typically when small cell carcinoma is within one lung, it’s considered limited; if it spreads beyond one lung, it’s considered extensive.
Small cell carcinomas can also sometimes secrete hormones, and that can lead to what is called paraneoplastic syndrome. One example is when the tumor releases an adrenocorticotropic hormone causing an increase in production and release of cortisol from the adrenal glands.
Causes
This causes what’s known as Cushing’s syndrome, which causes a number of symptoms, including elevated blood glucose and high blood pressure. Another example is when the tumor releases an antidiuretic hormone, which causes water retention leading to high blood pressure, edema, and concentrated urine.
A slightly different type of paraneoplastic syndrome is when small cell carcinoma prompts the body to produce autoantibodies that bind and destroy neurons causing the myasthenic syndrome, which is a type II hypersensitivity reaction.
Non-small cell carcinomas are more of a mixed bag in terms of where they usually arise. Just like small cell carcinoma, squamous cell carcinoma tends to be centrally located and has a strong association with smoking.
Smoking also increases the risk of adenocarcinomas, but they tend to develop peripherally, in a bronchiole or alveolar wall, Large cell carcinomas, and bronchial carcinoid tumors can be found throughout the lungs – centrally and peripherally.
Of these two, large cell carcinoma has a stronger link l to smoking. Both adenocarcinoma and squamous cell carcinoma can form Pancoast tumors, which are masses in the upper region of the lung that compress the blood vessels and nerves located there.
In particular, Pancoast tumors can compress and damage the thoracic inlet, brachial plexus, and cervical sympathetic nerves leading to their dysfunction and Horner syndrome.
Clinical symptoms of Horner syndrome include a constricted pupil, a drooping upper eyelid, and loss of ability to sweat on the same side of the body as the dysfunctional sympathetic nerve. A classic paraneoplastic syndrome associated with squamous cell carcinoma is the release of parathyroid hormone, which depletes calcium from the bones causing them to become brittle and increasing calcium levels in the blood.
And, finally, a paraneoplastic syndrome specific to carcinoid tumors is carcinoid syndrome which causes the secretion of hormones, particularly serotonin, which leads to increased peristalsis and diarrhea and bronchoconstriction causing asthma.
While non-small cell carcinomas tend to grow more slowly and be slower to spread than small cell carcinomas, the staging system is the same for both. It’s called “TNM” staging and represents three diagnostic categories: T, for tumor size and extent of local extension; N, for spread into nearby lymph nodes in the chest, particularly the mediastinum and hilar lymph nodes; and M, for metastasis to a secondary site.
Within each of these categories are sub-stages, T0-T4, N0-N3, and M0-M1, where an increasing number means increasing severity. Finally, the combinations of these sub-stages determine the stage group, assigned 0 to IV.
So for example, if the diameter of the tumor is less than or equal to 3 cm and not in the main bronchus has invaded the hilar lymph node on the same side of the chest, but has not spread outside the chest to other tissues, it’s categorized as T1, N1, M0 and can be considered stage group II. But if the tumor metastasizes to a secondary site, it’s considered M1, and staging group IV regardless of it’s T or N value.
Symptoms
Symptoms of lung cancer vary based on the size and location of the tumor, whether or not it has spread to other organs, and whether or not it generates hormones – all of which is often predicted by the type of cancer.
In response to the cancer cells, the body mounts an immune response, which results in the release of chemokines like TNF-alpha, IL1-beta, and IL-6, which can cause weight loss, fevers, and night sweats. If the primary tumor physically obstructs the airway and presses on surrounding tissue structures, it can cause a cough, shortness of breath, and leads to pneumonia in the lung tissue behind the obstruction.
Compression of nearby nerves can cause pain, and compression of specific nerves like the recurrent laryngeal nerve and phrenic nerves can cause changes in voice or difficulty breathing, respectively.
Compression of nearby vessels like the superior vena cava can cause a backup of blood in the face leading to facial swelling and shortness of breath. Finally, if cancer cells invade into a blood vessel, then mucus can get blood-tinged, or blood clots can get coughed up.
Diagnosis
Initially, lung cancer is usually identified as a coin-shaped spot, called a coin lesion on chest X-ray, or a non-calcified nodule on chest CT. Infections can also cause similarly shaped spots, so a tissue biopsy from bronchoscopy or a CT-guided fine-needle aspiration is typically done to make a histopathologic diagnosis.
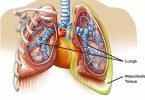
Also Read MESOTHELIOMA, Causes, Signs and Symptoms, Diagnosis, and Treatment.
Treatment
Though treatment will vary by category and stage of lung cancer, often a commonality is the use of surgery if appropriate, chemotherapy or immunotherapy, and radiation therapy when possible.
In general, the goal of surgery is to remove as much of a tumor, ideally all of it, and to have a small border of healthy tissue around it so that all of the cancerous cells are gone.
Depending on the size and location of the tumor, a small wedge of tissue may be taken, or up to an entire lung, in which case the airway is sutured shut to prevent air from leaking into the body cavity.
In addition, it’s typical to remove nearby lymph nodes that have metastasis and manage clinical symptoms.
Since pain is a significant chronic symptom of lung cancer, it’s often managed through both nonpharmacologic approaches like yoga and guided imagery, as well as pain medications.
So, a quick recap: Lung cancer is the uncontrolled growth of respiratory epithelial cells.
The minority are small cell cancers, and the cancers are that they can cause airway obstruction, compression of nearby nerves and the superior vena cava, cause paraneoplastic syndromes, and induce an immune response that causes symptoms like weight loss, fevers, and night sweats.
Overall, lung cancers have a high rate of metastasis to other organs and are treated with a combination of surgery, chemotherapy, immunotherapy, and radiation, depending on the situation.
[mashshare]

Leave a Comment